The diagnosis of Kawasaki disease among Nigerian children: a nightmare for the caregivers and the doctors
Introduction
Kawasaki disease (KD) also called Kawasaki syndrome (KS) or mucocutaneous lymph node syndrome is a febrile illness of childhood. It is a self-limited acute vasculitic syndrome of unknown etiology, first described by Kawasaki in 1967 (1). At that time, he reported 50 children from 1961–1967 who presented with a distinctive clinical illness characterized by fever and rash, which was then thought to be a benign childhood illness. It has worldwide occurrence but commoner in children form Japan, USA, Asian origin intermediate in non-Hispanic African Americans with an annual incidence of 112 cases per 100,000 children (2). Up to 6,000–7,000 new cases per annum has been reported in Japan and 10 per 100,000 in USA (3). KD is commoner in those <5 years (80%) peak of 18–24 months (2). Although recent reports have emphasized the occurrence of KD in older children, who may have a higher prevalence of cardiovascular complications related to late diagnosis (4). It is commoner in males (2). In the United States, KD is more common during the winter and early spring months (5).
The epidemiology of KD in developing countries is largely undefined although very few cases have been reported giving the impression that the condition is rare (6-9). A close differential of KD is measles which is common among children in Nigeria this gives the possibility that some cases might therefore have been misdiagnosed as measles. The apparent rarity of the disease may also be due to the low index of suspicion among Physicians and other healthcare workers in Nigeria. The current study highlights few cases seen among children in Lagos, Nigeria in various private and public hospitals over a period of five years. This aim is to enumerate the presenting features, challenges encountered in the management of the subjects, the outcome of the subjects and increase awareness of KD among health practitioners in the sub region.
Methods
These reported cases were seen in a public hospital and three private hospitals in Lagos State, Nigeria. Five of the cases were treated at the Lagos State University Teaching Hospital, Ikeja (LASUTH). Two cases were seen at Reddington Hospital and a case at Premier Hospital. The Lagos State University Teaching Hospital, Ikeja is a tertiary centre with referrals from different hospitals both public and private hospitals within and outside Lagos State. The Department of Paediatrics in this center has a well-established cardiology unit. Reddington Multi-Specialist Hospital and Premier Hospital are highly recognized standard private hospitals in Nigeria. Routine cardiac evaluation also takes place in these centres. All the cases had cardiac evaluation by a Paediatric cardiologist.
A prospective audit of patients that presented at the above centres with the diagnosis of KD from January 2011 to December 2016 were done. Diagnosis of KD made according to the diagnosis criteria by the American Heart Association. Serial complete blood count and where available, C-reactive protein were also done for the patients.
Transthoracic echocardiography was done in all by a Paediatric cardiologist using 2D machine with M-mode and Doppler facility to determine the presence of a cardiac involvement. Follow-up echocardiography was also done. Demographic data of the subjects including presenting clinical features, time of onset of fever to the time of diagnosis, use of intravenous immunoglobulin (IVIG), cardiac features and outcome were documented.
The study was approved by ethics board of the Lagos State University Teaching Hospital (NHREC04/04/2008) and written informed consent was obtained from all patients.
Data was analyzed using done using Microsoft Excel statistical software supplemented by statistical package for social sciences (SPSS) version 20.0. Probability values less than 0.05 were considered statistically significant.
Results
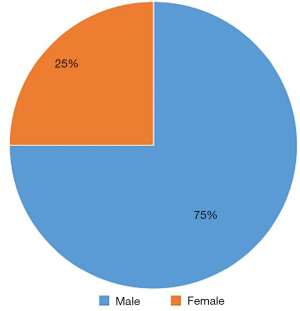
Eight cases seen were males with a male-to-female ratio of 3:1 as shown in Figure 1.
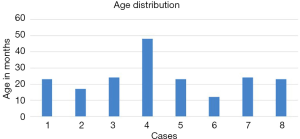
The median age at diagnosis was 23.5 months and age ranged of cases seen was between 12 and 48 months as depicted in Figure 2.
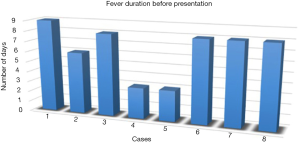
As shown in Figure 3 below, duration of fever prior referral to LASUTH or admission at the private hospitals ranged between 3 and 9 days. However, diagnosis of KD was made 9 days after the onset of fever.
Bilateral non-purulent conjunctivitis and oral cavity changes were seen in 7/8 (87.5%) of the cases. Cervical lymphadenopathy occurred in 3/8 (37.5%), polymorphous rash 6/8 (75%) and peripheral changes in 5/8 (62.5%) of cases.
Coronary artery abnormality (CAA) was observed in 3/8 (37.5%) cases. CAA was seen in both the complete and incomplete groups. Two (66.6%) of the cases with CAA had incomplete KD.
BCG scar reactivation as a clinical manifestation of KD was seen in a case (12.5%). The reactivation was seen in an incomplete form of KD.
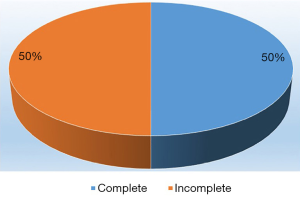
Equal number of subjects had complete and incomplete KD as shown in Figure 4.
There was raised erythrocyte sedimentation rate and C-reactive protein which are acute phase reactants in cases the investigations were done. Severe thrombocytosis of 800,000/mm3 was seen in a case as shown in Table 1.
Table 1
| Laboratory and radiological parameters | Case 1 | Case 2 | Case 3 | Case 4 | Case 5 | Case 6 | Case 7 | Case 8 |
|---|---|---|---|---|---|---|---|---|
| PCV (%) | 24 | 27 | 27 | 34 | 35.5 | 28 | 26 | 28.8 |
| WBC count/mm3 | 22,400 | 20,600 | 11,200 | 12,100 | 21,000 | 17,000 | 14,400 | 18,900 |
| Platelet count/mm3 | 519 | 248 | 414 | 800 | 655 | 575 | 414 | 489 |
| ESR (mm/hr) | 90 | 86 | 75 | 65 | 131 | 103 | 88 | |
| C-RP (mg/L) | – | 21 | – | 75.3 | – | – | 76 | – |
| ECHO | Normal | LCA dilatation | Normal | RCA dilatation with ventricular dysfunction | Normal | Normal | Normal | LCA and RCA dilatation |
PCV, packed cell volume; WBC, white blood cell; ESR, erythrocyte sedimentation rate; C-RP, C-reactive protein; LCA, left coronary artery; RCA, right coronary artery.
Discussion
The spectrum of eight cases of KD reported from various hospitals in Lagos over a period of five years aptly demonstrates the fact that the disease deserves the attention of regional clinicians. This is especially so due to the excellent outcomes achieved when appropriate and timely therapy is instituted (10). Prevalence values exist for black populations in developed countries like the United States of America (11), but not for Nigeria and indeed Africa as a whole, as revealed by careful literature search. There has been no national survey to determine the occurrence of KD in Nigeria as has been done in Japan (12).
Importantly however, the finding in this report of eight cases of KD over a period of five years suggest that the condition may be more prevalent in the region than the paucity of published data may suggest. Fewer than ten cases in total have been published in Nigeria since the first reported case by Ikpatt in Calabar in 1989 (6-9). KD is now reported to be the leading cause of acquired cardiac disease in Western countries (11). This should naturally have piqued the interest of stakeholders in the country with regards to making attempts to determine the contribution of KD to data on the most common causes of acquired heart disease in Nigeria.
There is reported to be a slight male preponderance in cases of KD. Of the eight cases reported here, six were males and two females giving a male: female ratio of 3:1, higher than the distribution pattern previously reported (13). On this series, patients’ ages ranged between twelve months to four years. This is in keeping with previous findings that most patients are under five years of age (14).
The American Heart Association criteria for diagnosis of KD requires the presence of a fever for a minimum of five days and at least four out of five principal criteria: extremity changes, polymorphous exanthema, bilateral bulbar conjunctival injection without exudates, lip and oral cavity changes and cervical lymphadenopathy (>1.5 cm diameter), usually unilateral (10
Two-thirds of the cases had polymorphous rashes. Polymorphous rash is reported to occur in about 70% to 90% of cases with KD (15). Bilateral non-exudative bulbar conjunctival injection and oral cavity changes which was present in all but one case is reported elsewhere to be present in at least 87.5% percent of cases (16).
Cervical lymphadenopathy (>1.5 cm diameter) was present at presentation in only 1 patient (8.75%) of the patients. This is lower than previously reported occurrence that ranged between 25% and 70% (16,17).
A well recognized clinical manifestation of KD which is however not included in the diagnostic criteria is the reactivation of a Bacille-Calmette-Guerin (BCG) scar, reported in up to 50 percent of patients who have previously received BCG vaccination (17). One patient in this series demonstrated this phenomenon. BCG scar reactivation has been suggested to be of high specificity in making a diagnosis of KD (18).
Two-third of patients in this series had been diagnosed as having other conditions and had been administered antimalarial and antibiotics accordingly with failure of symptoms to resolve. This highlights the fact that in this environment KD is only rarely considered as a likely diagnosis on initial evaluation of patients.
By far the most lethal complication of KD is the cardiac involvement of the disease. Cardiac manifestations are reported to develop in up to 25% of untreated cases of the disease (10). Three of the eight cases reported here had cardiac involvement, mainly coronary arterial aneurysms. It is noteworthy to add that with treatment, the three patients with coronary involvement initially now has normal sized coronaries on follow up and have no symptoms or signs of coronary disease. Long term follows up of these patients is on-going and the outcome will be addressed in further studies.
In the few reports published in Nigeria, the administration of IVIG, an established therapy for KD with excellent outcomes, was not reported on account of inaccessibility either due to high cost or logistic limitations (7-9). The cost of IVIG as at the time of management of the patients in this series went up from about three thousand United States of America dollars to five thousand seven hundred and fifty dollars (almost one hundred percent appreciation) but seven of the patients were privileged to have had access to it. The only one who could not receive the IVIG in Nigeria due to non-availability had to be flown abroad to receive this life saving treatment. Additionally, IVIG is available in only one center in Nigeria, once it is not available from this only source, the only option will be to source for it abroad; could this be responsible for the high price of this medication in Nigeria? For one of the patients, IVIG was not available in Nigeria, one of the parents had to fly to one of our neighboring country, Ghana to procure it. Effort to secure this drug in the neighboring country in the sub-region also proved abortive, hence patient had to be flown to England to receive the treatment. The index patient was fortunate to be able to afford such a treatment which is not within the reach of a common parent in Nigeria. The unavailability of IVIG in the neighboring country also is a pointer to the fact that this shortage is not limited to Nigeria only. This call for a need for governmental and non-governmental agencies in health not only in the African sub region but also in the developed world to make concerted efforts to make IVIG available and affordable in Nigeria and her sub-region. This will go a long way in limiting the morbidity and mortality from KD, allowing timely administration and thus prevention of the cardiac complications.
IVIG was given at 2 gram/kilogram to seven cases. Interestingly, three of these had cardiac manifestations which are dilatation of the coronary arteries with co-existence of ventricular dysfunction in a case. The administration of IVIG was after the first week of the onset of fever but within the first ten days of fever in these subjects. The three cases were admitted at a separate facility for management, and were managed for a different condition initially, introducing a ‘lag’ period before administration of IVIG. Complete resolution of symptoms was seen within 24 hours of administration of IVIG. All the three subjects with cardiac complications had normal echocardiographic findings on follow up.
Incomplete KD is an important clinical entity diagnosed when a patient has a fever persisting for at least five days but has fewer than the four principal criteria required for diagnosis. The risk of developing cardiac complications in incomplete KD is reported to be as high as in the classic form of the disease, making it potentially more dangerous as diagnosis seems more likely to be missed. Indeed, of the three patients with incomplete KD in this series, two of the subjects had aneurysms of the coronary arteries, lending credence to this suspicion. Further study along this line clearly must be pursued.
As alluded earlier, late presentation is more often the case in this environment as is demonstrated by this series. This seems to suggest the fact that there is not a high enough index of suspicion for KD in this environment. The consequences of late presentation can be catastrophic as cardiac affectation occurs in the sub-acute phase (2–6 weeks after onset) of illness.
KD occurs among Nigerian children; index of suspicion is low hence most are diagnosed late and hence receive intervention late. However, the outcome of KD among children in Lagos is good. All are well on follow up. IVIG is not readily available in Nigeria and when available is beyond the reach of a common man. There is a need for urgent interventions to reduce morbidity and mortality from KD among Nigerian children.
Acknowledgments
The patients described above and their parents are gratefully acknowledged.
Funding: None.
Footnote
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jphe.2017.06.06). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). The study was approved by ethics board of the Lagos State University Teaching Hospital (NHREC04/04/2008) and written informed consent was obtained from all patients.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Kawasaki T. Acute febrile mucocutaneous syndrome with lymphoid involvement with specific desquamation of the fingers and toes in children. Arerugi 1967;16:178-222. [PubMed]
- Yanagawa H, Nakamura Y, Yashiro M, et al. Incidence survey of Kawasaki disease in 1997 and 1998 in Japan. Pediatrics 2001;107:E33 [Crossref] [PubMed]
- Yanagawa H, Nakamura Y, Ojima T, et al. Changes in epidemic patterns of Kawasaki disease in Japan. Pediatr Infect Dis J 1999;18:64-6. [Crossref] [PubMed]
- Stockheim JA, Innocentini N, Shulman ST. Kawasaki disease in older children and adolescents. J Pediatr 2000;137:250-2. [Crossref] [PubMed]
- Chang RK. The incidence of Kawasaki disease in the United States did not increase between 1988 and 1997. Pediatrics 2003;111:1124-5. [Crossref] [PubMed]
- Ikpatt NW, Ibia EO. Mucocutaneous lymph node syndrome in Calabar--a case report. East Afr Med J 1989;66:776-81. [PubMed]
- Sotimehin SA, Ogunlesi TA, Adekanmbi AF, et al. Kawasaki Disease in a Nigerian child- a case report. Niger Med Pract 2010;57: [Crossref]
- Sani UM, Ahmed H. Kawasaki disease: an unusual presentation in a 14-year old boy in Sokoto, north western Nigeria. Niger J Paed 2013;40:422-5. [Crossref]
- Eno-Obong EU, Mkpouto UA. Kawasaki Disease in a two year old Nigerian child: full recovery with supportive treatment. Ibom Med J 2014;7:40-4.
- Newburger JW, Takahashi M, Gerber MA, et al. Diagnosis, treatment, and long-term management of Kawasaki disease: a statement for health professionals from the Committee on Rheumatic Fever, Endocarditis, and Kawasaki Disease, Council on Cardiovascular Disease in the Young, American Heart Association. Pediatrics 2004;114:1708-33. [Crossref] [PubMed]
- Nakamura Y, Yanagawa H. The Worldwide Epidemiology of Kawasaki Disease. Prog Pediatr Cardiol 2004;19:99108. [Crossref]
- Nakamura Y, Yashiro M, Uehara R, et al. Epidemiologic features of Kawasaki disease in Japan: results of the 2009-2010 nationwide survey. J Epidemiol 2012;22:216-21. [Crossref] [PubMed]
- Moore A, Harnden A, Mayon-White R. Recognising Kawasaki disease in UK primary care: a descriptive study using the Clinical Practice Research Datalink. Br J Gen Pract 2014;64:e477-83. [Crossref] [PubMed]
- Ozdemir H, Ciftçi E, Tapisiz A, et al. Clinical and epidemiological characteristics of children with Kawasaki disease in Turkey. J Trop Pediatr 2010;56:260-2. [Crossref] [PubMed]
- Fukushige J, Takahashi N, Ueda Y, et al. Incidence and clinical features of incomplete Kawasaki disease. Acta Paediatr 1994;83:1057-60. [Crossref] [PubMed]
- Harnden A, Takahashi M, Burgner D. Kawasaki disease. BMJ 2009;338:b1514. [Crossref] [PubMed]
- Seo JH, Yu JJ, Ko HK, et al. Diagnosis of incomplete kawasaki disease in infants based on an inflammation at the bacille calmette-guérin inoculation site. Korean Circ J 2012;42:823-9. [Crossref] [PubMed]
- Rezai MS, Shahmohammadi S. Erythema at BCG Inoculation Site in Kawasaki Disease Patients. Mater Sociomed 2014;26:256-60. [Crossref] [PubMed]
Cite this article as: Animasahun AB, Adekunle MO, Kusimo OY, Fadipe C. The diagnosis of Kawasaki disease among Nigerian children: a nightmare for the caregivers and the doctors. J Public Health Emerg 2017;1:69.